Getting treatment
PGP can be safely and effectively treated with hands-on individualised treatment, including manual therapy from a physiotherapist, osteopath or chiropractor.

Experienced osteopaths, chiropractors or physiotherapists can usually treat PGP safely and effectively with hands-on individualised treatment, including manual therapy.
PGP is treatable at any stage of pregnancy, or after your baby is born.
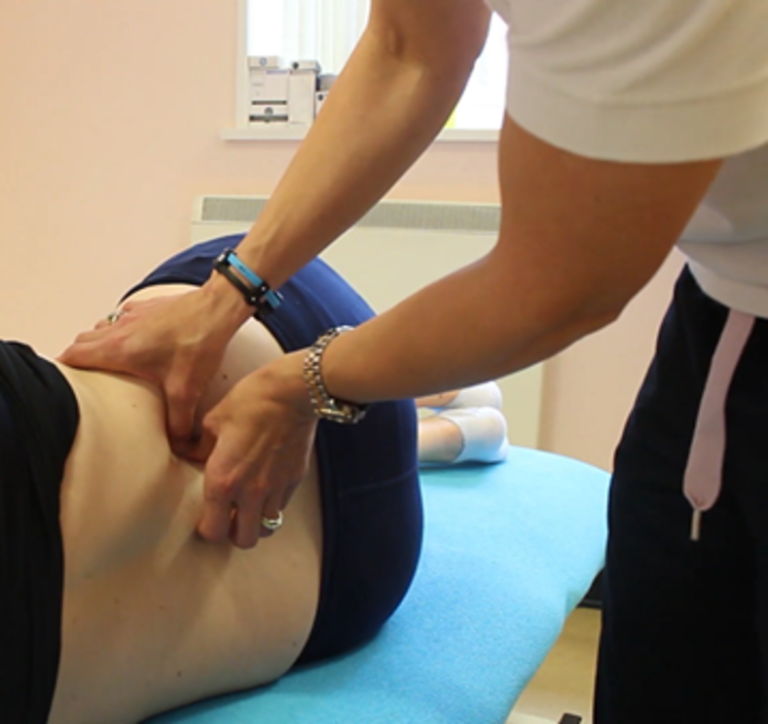
PGP can be safely and effectively treated with hands-on individualised treatment, including manual therapy from a physiotherapist, osteopath or chiropractor.
Exercises, mobility aids and pain-relieving medication can help you to manage some of the symptoms of PGP but they do not address the underlying cause of your pain, your pelvic joint dysfunction. Often, a high degree of pain prevents muscles from working properly so, regardless of how much you exercise, your muscles are unlikely to function correctly.
However, once your pelvic joints and muscles are treated with manual therapy and move more freely (normally), you should experience less pain. Exercises are important to help to strengthen the muscles supporting your pelvis, and mobility aids and pain relief can help to manage symptoms between treatments.
Ask your GP or midwife for a NHS physiotherapy referral.
In some areas this will mean a referral to a women’s health physiotherapist, in other areas you will be referred to a musculoskeletal physiotherapist.
You will normally be referred to the outpatient department of your local hospital or health centre.
Contact a local physiotherapist, osteopath or chiropractor to book an appointment if you are able to pay for private treatment. Different practitioners use different hands-on approaches to treat PGP.
If you have private medical insurance, you may be able to access an appointment through your insurance provider.
We have put together a list of recommended practitioners. These physiotherapists, osteopaths and chiropractors have all been recommended by at least 2 other women with PGP.
You can try your local sports injury clinic where you can ask to speak to a sports physiotherapist, who ideally specialises in pelvic joint problems, to discuss whether they have relevant experience. They don’t have to have specific experience in treating pregnant women. It is most important that they are confident at manually treating the pelvic joints and getting their patients back to playing sport and doing all the normal activities of daily life, rather than just coping with pain and avoiding normal activities. To find a manual or sports physiotherapist in your area visit the Physio First website.
You can contact your local osteopath or chiropractor – again, check that they have experience in treating pelvic joint problems. You may find these websites helpful: General Osteopathic Council, British Chiropractic Association and McTimoney Chiropractic Association.

Find a local private physiotherapist, osteopath or chiropractor to treat your pregnancy-related pelvic girdle pain (PGP).
Not all manual therapists have experience in treating PGP.
Whether you choose the NHS or private route, make sure your practitioner has looked after women with PGP before AND helped them.
Some women need to see more than one manual therapist before they find somebody who helps them. Don’t give up if the first one is not a good fit.
The practitioner you see needs to touch you. “Hands on” manual therapy – watch our Stickmum video to find out what to expect from treatment.
Not all GPs and midwives have up-to-date knowledge about PGP –take a copy of our ‘Stickmum’ leaflet with you to your appointment, and/or the National guidelines for PGP.
Unfortunately, many NHS and private manual therapists don’t know how to effectively treat PGP using manual therapy techniques.
If your PGP doesn’t improve after each treatment, then it is important to try another therapist, as you may not be receiving the best treatment available.
To understand why you might not be improving after manual therapy treatment, please visit our ‘What to do if treatment is not helping’ page.
Remember, if you are told:
Ask to be referred to someone who has experience treating PGP in pregnancy.
Medical knowledge is always evolving and so is our understanding of PGP. We now know that PGP is a treatable condition for most women. People who contact the Pelvic Partnership confirm that manual ‘hands-on’ therapy has helped them.
Unfortunately we are in a position where, without an increase in donations, we will only be able to continue to operate for another 4 months.
Donate today to help us help others with pregnancy-related pelvic girdle pain (PGP)